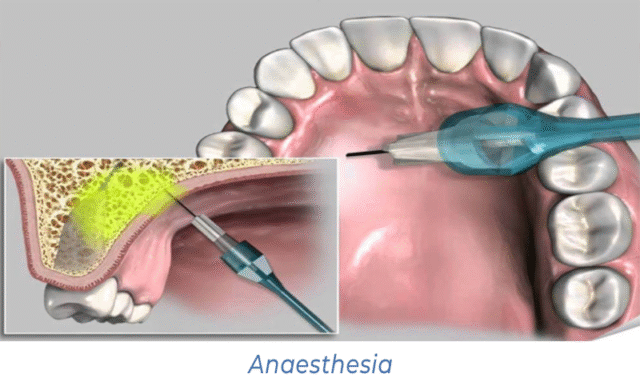
Local anaesthesia is an integral part of modern dentistry. Thanks to painkillers, doctors can perform surgical and therapeutic procedures without causing patients pain. However, like any medical intervention, anaesthesia is sometimes accompanied by complications or side effects.
According to the American Dental Association, serious complications are infrequent. For example, allergic reactions occur in only 0.01% of all cases of use, making it a very low-risk procedure for most patients.
Patients need to know which effects are considered regular and temporary, and which require specialist attention. The article explains this more.
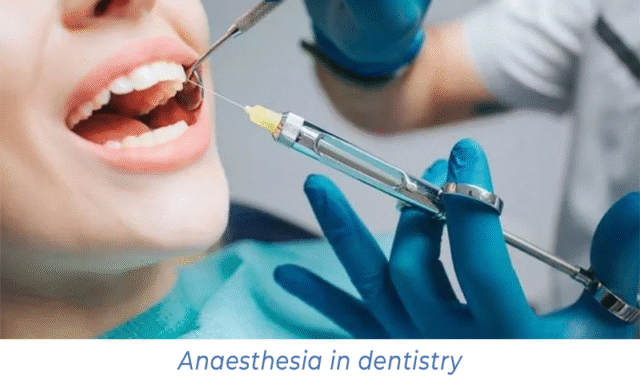
Local anaesthesia in dentistry and its importance
Modern drugs effectively block pain impulses while keeping the patient conscious. This ensures comfort and safety during caries treatment, prosthetics, implantation, or tooth extraction. The effectiveness of local anaesthesia for pain relief during routine procedures, such as caries treatment or tooth extraction, reaches 95-100%.
In some cases, medication-induced relaxation is also used with various types of sedation, which helps patients with increased anxiety or a pronounced gag reflex.
The dentist’s task is to perform the procedure with high quality and minimise the risks of side effects from anaesthesia.
Classification of complications after anaesthesia
Complications can be divided into two large groups:
- General complications are reactions of the whole body that are not limited to the area where the drug was administered. They are associated either with individual intolerance or with the systemic action of the anaesthetic. These include allergic and toxic effects, effects on the cardiovascular system, etc.
- Local — develop in the injection area and are associated with the technical features of anaesthesia. These include haematoma, pain and tissue swelling, paraesthesia and neuritis, etc.
Each group has its own causes and mechanisms of development.
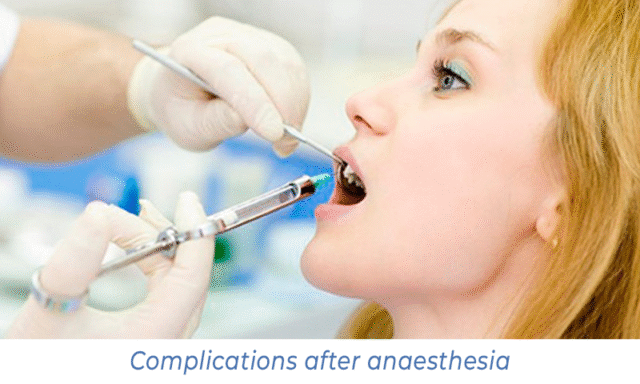
Common complications of local anaesthesia
Rare but possible complications include:
- Allergic reactions – from urticaria and Quincke’s oedema to anaphylaxis.
- Toxic effects – (dizziness, tremor, convulsions, cardiac arrhythmia) in case of accidental intravascular administration or overdose.
- Psychogenic reactions – fainting, drop in blood pressure, panic attacks.
- Idiosyncrasy is an individual’s unpredictable response unrelated to the dose.
- Effects on the cardiovascular system are tachycardia and arrhythmia (more common with adrenaline-containing drugs).
Such complications are rare and account for less than 1% of all cases, especially when dosage protocols and injection techniques are followed.
Local complications of anaesthesia and their causes
Local reactions are more common and are associated with the direct administration of the drug:
- Haematoma occurs when a needle damages a blood vessel.
- Pain and tissue swelling due to trauma or the solution entering dense structures.
- Infection due to non-compliance with sterility.
- Mucosal necrosis occurs when using a solution that is too concentrated.
- Paresthesia and neuritis – nerve damage or prolonged pressure of the anaesthetic on nerve fibres.
At the KES clinic, thanks to our doctors’ extensive experience and the use of modern protocols, the risk of local complications is minimal and rarely requires intervention.
Sometimes patients complain of numbness after a tooth filling. This is due to the prolonged action of the anaesthetic, which usually goes away on its own after a few hours.
Complications after mandibular anaesthesia
Mandibular anaesthesia is performed to numb the lower jaw. Possible complications:
- Temporary difficulty opening the mouth (trauma to the masticatory muscles).
- Nerve damage with short-term paraesthesia (numbness), occurring in approximately 1 in 26,000-150,000 injections. In 95% of cases, the numbness resolves within 8 weeks.
- Development of a haematoma in the area of the mandibular branch.
These complications are usually reversible and resolve with proper treatment.
Local complications of infiltration anaesthesia
Infiltration anaesthesia is most often used on the upper jaw. Possible reactions:
- swelling of the mucous membrane;
- a brief burning or pressure sensation;
- rare cases of the drug entering a blood vessel, which can cause pale skin or tachycardia.
Side effects and consequences of dental anaesthesia
The most common consequences are:
- temporary sensitivity impairment (numbness, feeling of ‘cotton wool lips’);
- difficulty eating until the anaesthetic wears off;
- possible microtrauma to the mucous membrane if the patient bites their lip or cheek during numbness.
If swelling occurs after the procedure or inflammation after tooth extraction, it is important to distinguish between a normal body reaction and a complication associated with infection or improper care.
Prevention of complications
Prevention of complications depends on both the doctor and the patient.
On the part of the dentist:
- careful collection of medical history (allergies, concomitant diseases);
- correct choice of dose and drug;
- compliance with the injection technique.
On the part of the patient:
- inform the doctor in advance about all chronic diseases and medications (collecting complete information about the patient’s health reduces the risk of complications by 80%);
- do not eat solid food until the anaesthesia has worn off;
- strictly follow care recommendations, including rules on how to treat inflammation after tooth extraction.
Complications after anaesthesia in dentistry are rare and, if diagnosed in a timely manner, do not pose a threat to health. Most side effects are temporary and go away on their own.
The KES clinic uses modern anaesthesia in accordance with international safety protocols. Our doctors’ experience and individual approach to each patient minimise the risk of complications and ensure the most comfortable treatment possible.