Periodontal disease treatment
WHAT IS THE DIFFERENCE BETWEEN PARODONTOSIS AND PERIODONTAL DISEASE?
WHAT IS PERIODONTITIS?
Periodontitis – is an inflammation of the gums and the teeth’ supporting structures and is one of the most common human diseases.
Periodontitis is caused by bacteria known as periodontal bacteria. Although these bacteria are naturally present in the mouth, they are only harmful when their amount increases dramatically. This happens when a layer of bacteria and food debris, that is, plaque, builds up and remains intact on the teeth, usually in hard-to-reach areas such as between the teeth.
Some bacteria can multiply, producing harmful waste products that stimulate the body’s protective inflammatory response. As the disease progresses, chronic inflammation leads to the destruction of the jawbone and teeth loss.
For many people, this is a gradual process that takes place over many years, and if it is detected and treated promptly, then periodontitis can be stopped.
PERIODONTITIS SYMPTOMS
• bad breath;
• teeth shifting;
• “longer” teeth (gum recession);
• pain.
Bleeding from the gums may be less noticeable in smokers due to the effects of nicotine on blood vessels, and therefore the disease process may be masked.
CAUSES OF PERIODONTITIS
A healthy mouth is inhabited by over 700 different types of bacteria, most of which are entirely harmless and live in harmony with the host. However, due to poor oral hygiene, bacterial deposits build up near the gums, forming plaque, and creating more favorable conditions for dangerous bacteria.
In all cases, periodontitis is caused by an accumulation of bacteria.
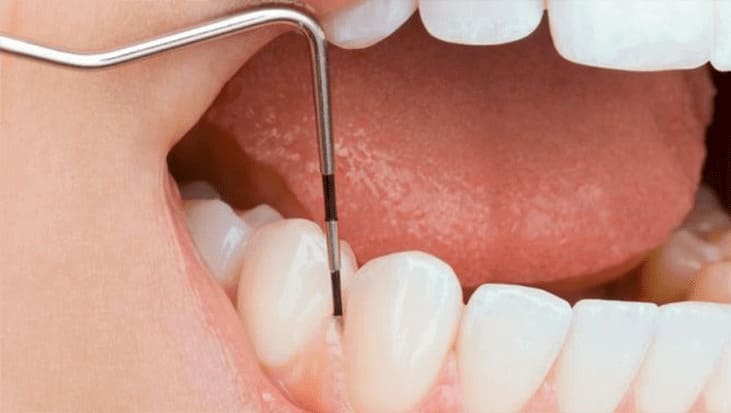
If plaque is not removed regularly, minerals are deposited into the plaque film over time, causing it to harden, turning into tartar. The presence of calculus encourages bacterial plaque growth towards the root of the tooth. As the inflammation progresses, the gums’ attachment to the root is disrupted, and a gap or periodontal pocket forms between them. This pocket is an ideal place for harmful bacteria to colonize and multiply, contributing to the development of the disease process. In their new habitat, bacteria produce toxic agents as products of their metabolism, which trigger the body’s defense mechanisms.
WHAT ARE THE CONSEQUENCES OF PERIODONTAL DISEASE?
Periodontitis is the leading cause of tooth loss.
If periodontal inflammation development does not stop, the supporting structures of the teeth, including the surrounding bone, are destroyed. Teeth weaken over time and fall out or need extraction. Painful abscesses and lengthening of the teeth with exposed roots may also appear due to gum recession.
COMPLICATIONS
- osteomyelitis of the maxillofacial apparatus;
- ulcerative erosive gingivitis;
- periodontitis, periostitis;
- alveolar pyorrhea – suppurating dental pockets;
- retrograde pulpitis;
- rampant caries;
- lymphadenitis.
It can cause gastrointestinal complications as well. Bacteria get into the stomach with saliva. The pus discharge can penetrate various organs and systems with the blood flow. Research results confirm that when tooth loss from periodontal disease occurs, the pathological process has already managed to cause irreversible harm to the body. Periodontal disease causes complications not only from the dentition but also has life-threatening consequences.
Untreated periodontal disease can affect overall health; for example, it creates an increased risk of complications during pregnancy (preeclampsia, premature birth, and low birth weight) and an increased risk of cardiovascular disease and diabetes.WHAT ARE THE RISK FACTORS FOR PERIODONTITIS?
Periodontitis progresses much faster and with more rapid tooth loss in smokers. Of 100% of periodontitis cases that do not respond to treatment, about 90% are smokers.
HOW IS PERIODONTITIS TREATED?
• neodymium laser. Laser therapy for periodontitis is non-traumatic and painless, has a high disinfecting and biostimulating result;
• injection treatments with the patient’s plasma.
TREATMENT TACTICS
- professional ultrasonic teeth cleaning;
- tooth decay treatment, extraction of the decayed roots;
- extraction of teeth that cannot be treated;
- splinting – strengthening the root structure with special fasteners;
- hyaluronic acid injection;
- drug therapy: hormonal, anti-inflammatory, regenerative, anaesthetics, styptic agents, and antibiotics.
Vitamin-mineral premix is prescribed. When the real cause is identified, drug therapy aims to prevent relapse and further develop pathology.
Antibiotic therapy affects the entire body, prevents the development of distant infectious foci, abscess, sepsis, osteomyelitis, and other purulent processes. Broad-spectrum antibiotics are active against many gram-positive and gram-negative bacteria.
Besides antibiotics, local therapy is indicated: rinsing the mouth with water-based chlorhexidine, nitrofurazone, iodinolum, ointments, and gels with antiseptic and regenerating effects.
Injection Therapy
- biogenic stimulants;
- hyaluronic acid;
- aloe extract;
- nicotinic acid and vitamin C;
- methyluracil;
- antibiotics;
- ribonuclease;
- own blood plasma etc.

It is essential to understand that the treatment of periodontal disease is complicated. Patients need not only medication but also physiotherapy treatment. The latter method enhances the effect of conservative therapy and includes the following measures:
Darsonvalization. The procedure assumes exposure to alternating currents of various frequencies. Darsonvalization stimulates blood supply, relieves pain, and reduces the sensitivity of the oral cavity. The general course of treatment is 30 procedures, 10-15 minutes each.
Laser therapy. It suppresses the infectious and inflammatory process, regenerates periodontal tissues, relieves swelling, itching, stimulates blood circulation and lymph flow.
Vacuum treatment. The use of vacuum prevents atrophic processes, enhances blood circulation and lymph flow, and has a mechanical contractile effect on muscle structures. The main goal of vacuum therapy is to stimulate the periodontal capillaries.
Electrophoresis with various drugs, gum massage (manual or mechanical) has an excellent effect. Proper massage enhances blood flow, accelerates healing, and stimulates normal lymph flow.RE-ASSESSMENT

