Pulpitis Treatment
Cost of treatment
Pulpitis
Pulpitis is an inflammation of the pulp due to a complication of dental caries caused by microorganisms and their products. Pulpitis can occur as a consequence of trauma, neglected erosion of enamel and dentin, iatrogenic conditions, or idiopathic causes.
Pulpitis is a common dental disease found in 20-25% of patients with oral pathologies. The disease affects both the molars and primary teeth.
Pulpitis is an inflammatory process of the tooth pulp, most often caused by streptococci and staphylococci.
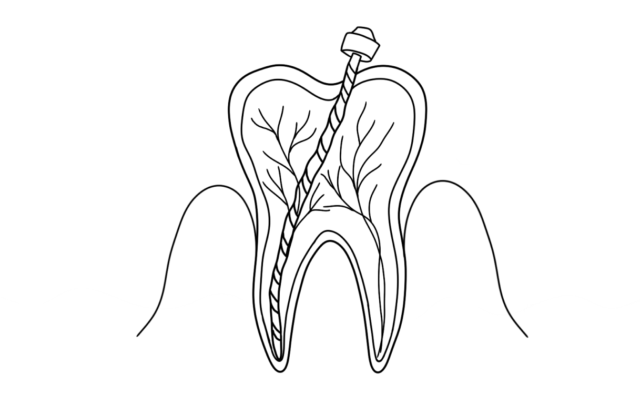
Causes of the disease
- advanced caries, poor-quality filling – pathogenic microorganisms penetrate the carious cavity, and their toxic waste products lead to the development of inflammation;
- streptococcal sore throat;
- tooth injuries – enamel chipping, fracture of a dentition element with pulp injury;
- pathological abrasion of dentition elements.

Forms of dental pulpitis
Pulpitis is classified according to various criteria. To establish the diagnosis, dentists use the International Classification of Diseases to Dentistry and Stomatology.
Types of pulpitis:
- Acute – serous limited or diffuse, focal sero-purulent.
- Purulent – a severe form of pathology accompanied by various complications.
- Chronic forms.
Sometimes lime deposits form in the pulp, which are painless; the dentist detects denticles during endodontic treatment.

How Is Pulpitis Treated?
In treating pulpitis, they try to fully or partially preserve the pulp and restore the tooth’s functionality, so conservative methods are used. In advanced cases, it is necessary to remove the pulp.
Without proper and timely treatment of pulpitis, pulp necrosis, periodontitis, periostitis, and osteomyelitis develop.
Complications can arise during the treatment of root canals of teeth – breakage of the instrument inside the canal, perforation of the bottom or walls of the tooth cavity. Negative consequences can occur due to non-compliance with the rules for using temporary pastes extruding the filling material beyond the upper part of the root.
Pulpectomy – removal of the entire pulp, used in treating all types of pulpitis.

How Does a Doctor Diagnose Pulpitis?
If you have signs of pulpitis, you should visit a dental clinic. The doctor makes a diagnosis based on a checkup, analysis of patient complaints, and imaging.
Signs of pulp inflammation on examination:
- the carious tooth with altered dentin;
- the affected element reacts painfully to temperature changes;
- percussion is painful.
The dentist conducts a differential diagnosis to exclude deep caries and chronic periodontitis. Additionally, a consultation with a neurologist may be required to exclude trigeminal nerve damage, and the patient may need an ENT specialist if suppurative otitis media or sinusitis is suspected.

FAQ
Are root canals treatment painful?
Currently, all dental procedures possibly causing painful sensations are performed under anesthesia. You do not need to worry and tensely expect that the doctor is about to “touch the nerve,” local anesthesia helps not think about the sensations during the procedure.
Root canal vs. extraction: what’s the difference?
Root canals are located within the roots of the teeth, holding them in the jaw. The roots remain, and the canals inside of them are cleaned and sealed.
Why do I need root canal treatment if my tooth doesn’t hurt?
It is not uncommon to have the canals re-treated due to poor previous treatment. The resealing can occur after the treatment, causing root canal infection, making periodontal disease visible through an X-ray. Modern standards of primary root canal treatment almost eliminate the need for further retreatment.
Earlier, during root canal treatment, a doctor would replace the medication inside the tooth, but how is it treated now?
The root canal treatment method requiring a change of medication for more than 4 weeks is hopelessly outdated. 1-2 visits are enough for most endodontic treatment cases.