Modern dental implantology shows stable results—about 98-99% of all implants placed successfully fuse and last for decades. But a small percentage of patients still experience treatment failures and rejection of the titanium implant. This article explains why this happens, whether a dental implant can be saved, and how to reduce the risk of complications.

Why might an implant fail to engraft?
Before we look at the reasons for treatment failure, we need to understand the terminology. Dental implant engraftment (osseointegration) is understood as its firm fusion with the jawbone. After that, the titanium screw completely replaces the function of the tooth root and serves as a reliable support for the prosthesis.
The process of engraftment lasts about 4-6 months and depends on various factors:
- the condition of the bone tissue;
- the material and design of the prosthesis;
- the technique of the surgery;
- the patient’s general health.
There are many reasons why dental implants do not survive.
Medical and anatomical reasons
The condition of the dentoalveolar system and the patient’s medical history play an important role. Problems after dental implant surgery are often related to factors such as:
- insufficient height and width of the jawbone as a result of progressive bone atrophy;
- low bone density due to osteoporosis;
- bite abnormalities and other associated dental problems;
- presence of poorly controlled diabetes mellitus or autoimmune diseases;
- old age, when there is a physiological decrease in the regenerative potential of tissues.
Placement errors and inadequate diagnosis
The success of dental implant surgery depends mainly on the skill of the doctor who plans and performs the surgery. Inattention or insufficient qualification of the doctor may lead to medical errors. They can occur both at the examination stage, if the dentist conducts an incomplete examination without a 3D CT scan and a full set of analyses, and in the course of the operation if the protocol of surgical manipulations is violated.
Possible causes of dental implant rejection:
- incorrect choice of size and design of the titanium screw;
- improper choice of the place and angle of placement of the structure into the bone tissue;
- overheating of the bone during the formation of the implant socket;
- traumatisation and compression of bone tissue during inaccurate insertion of the titanium screw;
- damage to the surrounding soft tissues during careless manipulations;
- failure to observe the rules of antisepsis.

The risk of complications increases in the case of immediate implant placement. This method shortens treatment time and minimises tissue damage. Still, it requires good oral hygiene and a satisfactory state of health. If the doctor ignores these conditions and does not conduct a thorough preoperative examination of the patient, the implant may fail.
Patient actions after the surgery
Even if a person has no restrictions on implants and the doctor has performed the surgery to the highest standards, this is not a 100% guarantee of success. After grafting a titanium implant, a period of rehabilitation begins, which should be treated very responsibly. Suppose the patient does not follow the doctor’s recommendations. In that case, they have an increased risk of complications and rejection of the implant.
The problems of the post-surgery period are mainly related to poor oral hygiene, trauma to the implant from hard food, and the inability to give up bad habits, such as smoking and drinking alcohol.
The reason for titanium implant rejection can be the patient’s refusal to take prescribed medications or ignoring scheduled visits to the dentist. All these factors increase the likelihood of peri-implantitis—inflammation of the tissues around the screw. It disrupts osseointegration and contributes to the loss of the titanium implant.
How do I know if an implant has failed?
Signs of dental implant failure can occur at different times, from a few months to several years after surgery. Suppose the problems are caused by medical errors or non-compliance with the rehabilitation rules. In that case, they usually manifest themselves in the first weeks after implant surgery. Symptoms of poor implant engraftment include:
- severe pain in the area of surgical intervention;
- significant swelling of the gum and cheek on the implant side;
- redness or lividity of the mucous membrane around the implant;
- purulent, oozing or bloody discharge from under the gingiva;
- bad, putrid breath odour;
- mobility of the implant;
- increased body temperature, weakness and other general signs of malaise.
Do not forget that soreness, swelling, and slight bleeding are natural reactions after surgical manipulation. Normally, they pass in 3-5 days and do not significantly affect the patient’s quality of life. If such symptoms last longer than 5-7 days and increase over time, they indicate postoperative complications.
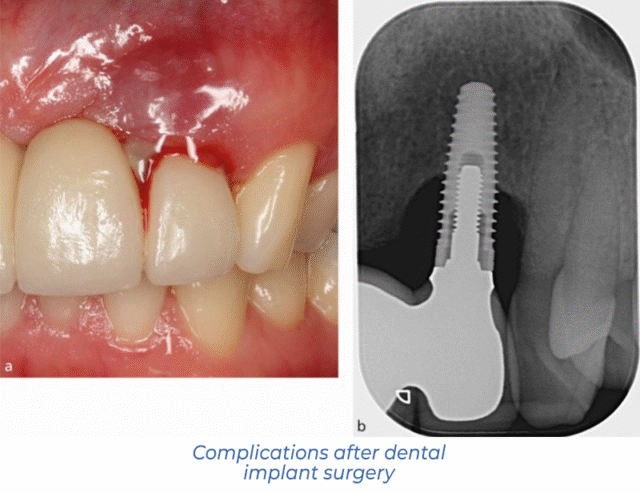
What should I do in case of implant rejection?
If the above symptoms appear, the patient should immediately contact the dentist who performed the surgery. It is not worth delaying a visit to the doctor. Delaying increases the risk of implant prolapse and the development of inflammatory processes.
Diagnosis: CT scan, X-ray, examination
For successful treatment, the dentist must understand why the dental implant has not fused. The doctor begins the appointment by clarifying the patient’s complaints and examining the oral cavity, during which he assesses local signs of inflammation.
Next, they will refer the patient for dental X-rays or a high-precision CT scan. The resulting images show the condition of the tissues around the tooth implant and allow for a correct diagnosis.
Medication or extraction
When implant complications occur, there are two courses of action available: conservative treatment or removal of the titanium screw. In the early stages, dentists use non-surgical methods: antiseptic treatment of the surgical site, removal of bacterial plaque, and physiotherapy. To eliminate peri-implantitis, antibiotic therapy and anti-inflammatory drugs are prescribed.
In case of deep spread of infection or complete rejection of the implant, surgical intervention is required. The dentist removes the titanium construction, treats the bone cavity, and prescribes local and systemic drugs. In case of bone atrophy, the doctor may prescribe different types of osteoplasty, and in case of soft tissue lesions, gingivoplasty.
Re-implantation: conditions and terms
Failure of treatment is not a reason to abandon the reconstruction of the smile. After the elimination of inflammation and the causes that led to the rejection of the implant, a repeat procedure is possible. It is performed under the following conditions:
- complete tissue regeneration in the area of titanium screw placement;
- sufficient volume and density of the jawbone;
- good hygiene and absence of inflammatory diseases of the oral cavity;
- stable general health of the patient, stable remission of chronic diseases;
- patient’s awareness and willingness to follow all the recovery period rules.
The soft tissues fully recover after the implant is removed and the new implant is inserted, which takes about 3-6 months. If bone grafting has been performed, implants will have to be postponed for 6-12 months.

Can failure to engraft be prevented?
Unfortunately, it is impossible to rule out all factors that affect treatment success. However, most causes of titanium screw rejection are due to patient or doctor errors that can be avoided.
For the implant to engraft, it is necessary to:
- choose the clinic and the doctor who will perform the procedure carefully;
- do not hide your medical history, bad habits and other individual risk factors from the dentist;
- prepare thoroughly for implant surgery: take all tests, adjust your lifestyle, treat your teeth and periodontal diseases;
- follow the dentist’s recommendations after the implant procedure, perform good oral hygiene and follow a gentle oral hygiene routine;
- do not miss planned visits to the clinic to examine the oral cavity and monitor the success of treatment.
Only joint work and trust between the doctor and the patient can ensure the long-term result of implant surgery—a beautiful and functional smile. At the KES Clinic, we take an individual approach to each case and offer full medical support at all stages of treatment.
 (66)
(66)