Dental implants from the Swiss manufacturer Nobel Biocare have been produced for over 50 years and are considered one of the best on the market. In Ukraine, premium-class products from Nobel and more low-cost options from Alpha Bio, a subsidiary of Nobel Biocare, are available for smile reconstruction.
In 99 patients out of 100, they successfully integrate (osseointegrate) and last for decades or even a lifetime. High osseointegration rates result from the special design of implants and the skill of dentists who select and place them.
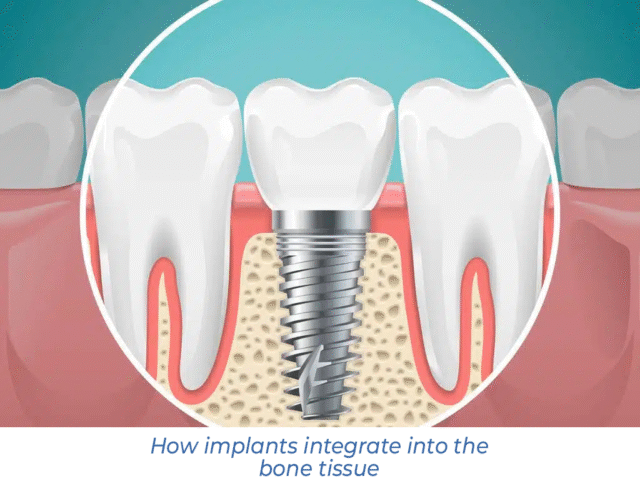
How Does Bone Affect Osseointegration?
Dental implant healing is the most important stage of treatment. The success of osseointegration determines the stability of the entire implant structure, the patient’s comfort, and the product’s lifespan. This process occurs due to the bone’s natural ability to regenerate—to recreate new, strong tissue in the area of damage. Therefore, the structural and functional state of the jawbone plays a decisive role in implant treatment.
Why is bone density important?
Sufficient bone volume is a prerequisite for any dental implant technique. Firstly, it allows for primary stability at the time of implantation of the titanium structure. The dental implant will be securely fixed if the bone has a high density and good thickness. The piece will loosen and shift if the bone tissue is fragile and porous. This can lead to complications and even rejection of the artificial root.
Secondly, a strong bone is necessary for osseointegration. The better the condition of bone tissue, the more mineral substances, organic components, and special cells, such as osteoblasts. All these elements participate in the process of implant engraftment. In osteoporosis or bone atrophy, osseointegration will be delayed and ineffective.
How does the bone interact with the implant?
The soft tissue heals in the first weeks after the Nobel Biocare or Alpha Bio implant placement, and bone-forming cells migrate to the injury site.
Osteoblasts synthesise organic fibres that form the matrix of future bone tissue. Then mineralisation occurs — the deposition of calcium salts responsible for bone strength. Osteointegration takes about 4-6 months. After completion, the implant is firmly connected to the jaw and functions almost like a natural tooth root.
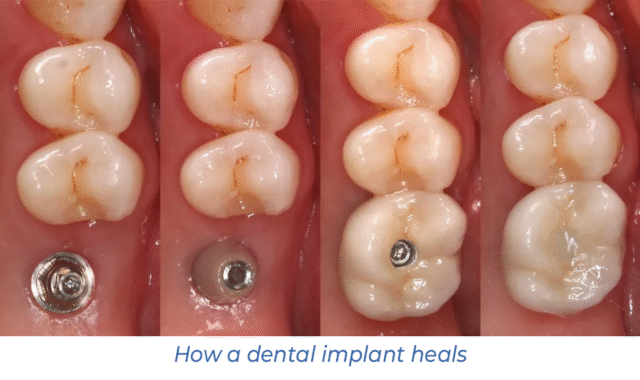
Nobel and Alpha Bio for Different Bone Types
To enhance implant results, manufacturers are improving the shape of the product and its surface:
- Nobel Biocare implant has an ultra-hydrophilic roughened surface called TiUltra, the topography of which changes from the neck to the top of the titanium structure. This ensures rapid and uniform bone growth around the implant, even in difficult clinical situations.
- Alpha Bio implant has a nanohydrophilic NiNA™ surface, which increases the contact area with the bone and accelerates and improves osseointegration processes. The product also has double microthreading for good primary stability.
How to choose an implant for dense bone?
If the bone tissue is in good condition, there are no special requirements for the choice of implant. Any Nobel Biocare or Alpha Bio options will suit such patients, as they are all high-quality.
When choosing a model, the dentist pays attention to the place of implant placement (frontal or chewing area), anatomical features of the jaw, and the intended method of prosthetics.
What to do in case of bone tissue deficiency?
In case of low bone volume or insufficient bone density, the implant must fulfil the following requirements:
- A cone-shape that ensures easy insertion and correct load distribution on the jaw;
- Deep and/or double threading, which allows the product to be firmly fixed even in fragile bone;
- The rough surface has a large contact area with bone tissue and facilitates osseointegration.
In case of severe atrophy in the upper jaw, dentists can use a special type of product—Zygoma zygomatic implants from Nobel Biocare. They are twice as long as conventional units and designed for fixation in the zygomatic bone. Such products are characterised by high primary and secondary stability. They are suitable for complete dentures according to the protocols All-on-4 and All-on-6.
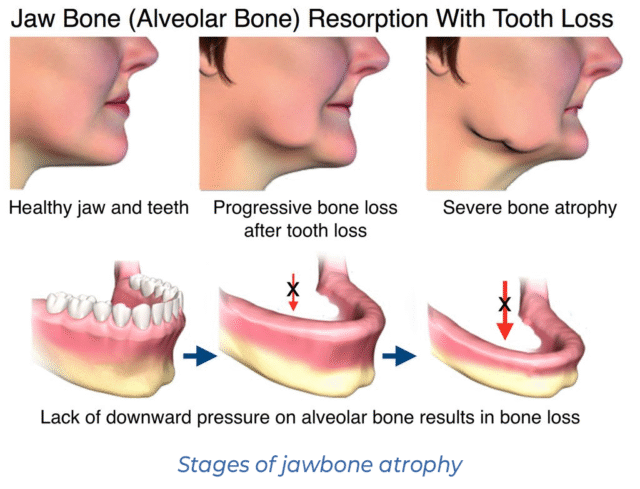
Diagnostic Methods Before Implant Surgery
An examination is a key step in preparing for implant treatment. Based on the diagnostic results, the dentist assesses the condition of the jawbone, identifies hidden diseases of the dentoalveolar system, and selects the type of implants and their placement sites.
3d computer tomography is recognised as the most accurate and informative method. It gives a three-dimensional image of the jaw and allows the doctor to plan the surgery using special software. A panoramic image of teeth (orthopantomogram), a targeted image of a diseased or destroyed tooth, and intraoral scanning are also used in dentistry.
Patients with jaw atrophy may be prescribed tests for vitamin D and bone metabolism markers to select the right tactics for preparing for implantation.
Bone Repair Options
Sometimes, dentists perform implant surgery without prior bone grafting in cases of insignificant atrophy. In this case, narrower and shorter implants are used, which can be placed without complications and the risk of damaging neighbouring tissues. However, most patients with bone atrophy will require special preparation for tooth reconstruction.
Bone grafting before implant placement
Osteoplasty is the main way to restore the jawbone. It is performed simultaneously with implantation or as an independent procedure 6-9 months before implants are implanted. For bone reconstruction, the following procedures are used:
- Sinus lift surgery;
- 3D-reconstruction based on the F. Curie method;
- Alveolar ridge splitting;
- Autotransplantation of bone tissue;
- Targeted tissue regeneration;
- Bone grafting with synthetic osteogenic material or donor bone material.
Each method has its own indications, advantages and disadvantages. The method of osteoplasty is discussed individually during a consultation with a surgeon.
How to increase bone density without surgery?
Conservative therapy can not completely restore atrophic bone. However, it slows down tissue destruction, accelerates metabolism, stimulates regenerative processes and improves implant success. The main treatment options are:
- A diet high in protein and calcium;
- Nutritional supplements with vitamin D, calcium and phosphorus;
- Antiresorptive drugs – bisphosphonates, which help with osteoporosis;
- Monoclonal antibodies (denosumab), which prevent bone breakdown;
- Synthetic analogues of calcitonin, a thyroid hormone that affects phosphorus-calcium metabolism.
A physician should prescribe any drugs to improve bone metabolism. Drug therapy combined with osteoplasty can help achieve the best results of implant surgery.
Factors that accelerate implant recovery
The placement of quality Nobel Biocare and Alpha Bio products is not the only way to increase the chances of treatment success. The procedure is also important. Navigation surgery, 3D planning, and minimally traumatic one-stage implant protocols all contribute to implant recovery.
Osteointegration largely depends on the conditions of the rehabilitation period and the patient’s willingness to follow the doctor’s recommendations. For the implants to take root faster, it is advisable to:
- Stop smoking and drinking alcohol;
- Follow a balanced diet with a high level of protein, vitamins and microelements;
- Avoid eating too hard food, which can traumatise the tissue around the implant;
- Perform daily oral hygiene routine at home;
- Avoid excessive physical activity and heat (bath, sauna).

In modern dentistry, plasmolifting is used to improve osseointegration. The patient’s blood plasma is enriched with platelets and growth factors and injected into the peri-dental tissues. It activates regenerative processes and accelerates the formation of new bone tissue.
Complications and Prevention
The risk of complications after implants from Nobel Biocare and Alpha Bio does not exceed 1-3%. Possible consequences of the surgery:
- Early complications – increasing pain syndrome, severe swelling, bleeding;
- Traumatisation of the maxillary sinus and branches of the trigeminal nerve;
- Postoperative wound infection;
- Peri-implantitis – inflammation of the tissue around the dental implant;
- Rejection of the dental implant.
To avoid negative consequences, it is recommended that you take medications prescribed by the doctor, rinse the mouth daily with antiseptics, and avoid traumatising the surgical area. If you experience any alarming symptoms, you should visit a dentist as soon as possible to find out the causes of the problem and start the necessary treatment.
 (169)
(169)



