Services
Dental implantation
WHAT IS AN IMPLANT?
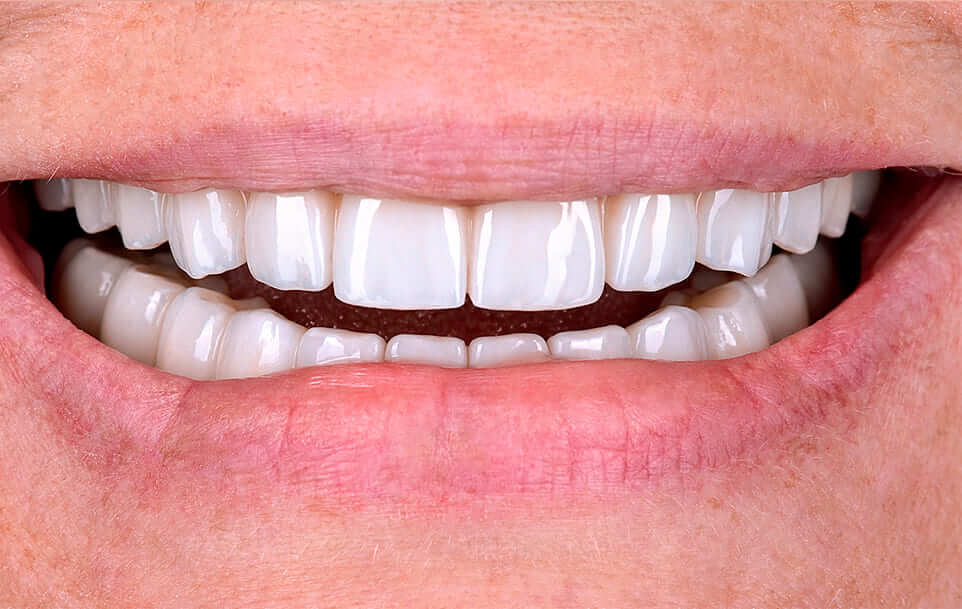
A dental implant is an artificial construction that replaces the root of a missing tooth; it is anchored in the upper or lower jaw’s bone tissue. Dental implantation can serve as a support for crowns, as well as removable and fixed restorations.Dental implants are the most natural-looking replacement for healthy, natural teeth. They allow living the life you want – to eat with confidence, smile, laugh, talk and enjoy all your daily activities without worrying about your teeth.

STAGES OF IMPLANTATION
When dental implants are placed in the jawbone (A), they fuse with your natural bone and become a solid foundation to support one or more artificial teeth called crowns.Abutment (B) – Placed over a dental implant to support your crowns.
Crowns are made in a dental laboratory using previously taken impressions (C).

THE BENEFITS OF DENTAL IMPLANTATION
Implantation in the hands of an experienced dentist and proper planning is one of the safest and most predictable dentistry procedures.
Modern dental implants have been successfully used for over 50 years.
CONTRAINDICATIONS TO DENTAL IMPLANTATION
Severe general illnesses such as diabetes, cardiovascular diseases, liver and kidney diseases, neoplastic diseases during chemotherapy or radiation therapy are critical contraindications.
Dental implantation is a relative contraindication for heavy smokers who are not ready to quit smoking and alcohol and drug abuse. The same applies to severe mental illness.
Dental implantation is a relative contraindication for heavy smokers who are not ready to quit smoking and alcohol and drug abuse. The same applies to severe mental illness.
Pregnancy and breastfeeding are contraindications for dental implants.
The process of bone growth must be completed. This usually applies to women aged 18 and men 20.
The process of bone growth must be completed. This usually applies to women aged 18 and men 20.
The generally accepted absolute contraindications for the artificial dental implants placement include:
- masticatory muscles hypertonia and bruxism;
- decompensated diabetes mellitus;
- severe mental disorders;
- functional failure of the liver and kidneys;
- bone mineralization disorder (osteoporosis);
- coagulation disorder.
In addition to absolute ones, there is a list of relative contraindications that do not exclude the possibility of implant surgery but suggest postponing it for a certain period. These contraindications include:
- carious lesions;
- low bone volume, which does not allow the implant placement;
- tartar;
- malocclusion;
- neoplasms in the oral cavity (granulomas, cysts);
- an inflammatory process in the soft tissues of the oral cavity;
- periodontitis, periodontal disease, and other gum diseases;
- tobacco smoking, if a person smokes more than one pack of cigarettes a day;
- pregnancy and breastfeeding;
- infectious and inflammatory diseases of a viral, bacterial, or fungal nature;
- physical fatigue;
- high risk of facial trauma due to extreme sports.

Book online
ALL-ON-4 CONCEPT
The All-on-4 concept provides our patients with a fixed prosthetics immediately after dental implantation

The advantages of this implantation concept allow:
- a full arch denture to be stabilized with just four implants;
- avoid bone grafting;
- carrying out the procedure in one stage since immediate loading is useful and shows the result;
- using fixed prosthetics, which are more suitable both in service and care, compared to the removable ones;
- this method has been scientifically proven to be effective.
INTERESTING FACTS ABOUT DENTAL IMPLANTS:
Dental implants are the only option for restoring missing teeth that preserve natural bone from atrophy (physiological bone loss after tooth extraction).600 AD
Ancient dental implants were discovered around 600 AD in the jaw of a Mayan woman. In 1952
The Swedish orthopedic surgeon P.I. Branemark discovered that titanium naturally fused with the bone and was one of the first to install titanium implants. 3 000 000
Today, 3 million people in the United States have implants, which is growing by 500 thousand annually. COMPLICATIONS AFTER DENTAL IMPLANT SURGERY
Dental implant failure is an immediate complication that appears after dental implant surgery. It is estimated that the complication prevalence rate is from 1.5 to 3% in patients undergoing this procedure. Initially, when the failure occurs, it causes an inflammatory response which leads to jaw bone destruction.
Tobacco smoking is an example of predisposing patient-dependent factor. Constant contact between the surgical site and the components of tobacco smoke will provoke an implant failure. Regular alcohol consumption can also affect indirectly.
Other potential reasons for the implant failure include:
1. Endogenous or exogenous infection of surgical site.
2. The immune response to a foreign body leading to implant failure.
3. Features of dentoalveolar structure.
4. Reduced local or common immunity and immune deficiency.
Other potential risk factors associated with possible implant failure include endocrine disorders, periodontal pathology, bruxism, and prior radiation therapy.
Сost of implants
Implant surgery with Alpha Bio Tec system, Israel
₴15,300
“Alpha Bio” implant + gum former + abutment + zirconia crown with screw fixing (completely prepared tooth)
₴32,800
1. Is there an age limit implant surgery?
There is no age limit. One of our patients, whose all 5 implants survived and still function properly, is 84 years old. This age is absolutely normal for treatment in European countries if the patient has no contraindications for implantation.2. How soon after tooth extraction can you have an implant?
We place implants in 6-8 weeks or 4 months after tooth extraction, depending on the bone volume loss.3. Can implants last a lifetime?
The success rate after implant surgery is over 99%. With proper care and regular oral hygiene routine that we tailor after implantation, they can last a lifetime.4. What are the indications for dental implant treatment?
An implant is a great solution when a single tooth or posterior teeth are missing, with complete loss of teeth in the upper and lower jaws. There is no age restriction for implants.5. Does dental implant surgery hurt?
It doesn't hurt more than any other dental treatment. Implant surgery is performed under local anesthesia; it can also be performed under sedation (a sleep-like state) or general anesthesia optionally and due to medical reasons.6. What are medical contraindications to implant therapy?
The main absolute contraindication to implant therapy is radiotherapy. Relative contraindications can be osteoporosis, diabetes mellitus, thyroid diseases, nervous and mental diseases, severe cardiovascular diseases.In these cases, the question of implant therapy is considered individually.7. How often do dental implant fail?
Official statistics indicate that a correctly placed implant survives in 98.5% of cases. Based on many years of experience in implant therapy, we give 98-99%.8. What if the patient is allergic to the implant material?
According to the German Association of Oral Implantology, an allergy to titanium, from which the implant is made, occurs in one out of 10,000 patients. In this case, we can carry out the LTT (Lymphozyten Transformation) allergy test. If titanium allergy is confirmed, we recommend using the less popular but effective zirconium implants.9. How many implants do I need?
With a single missing tooth - 1 implant, with the loss of posterior teeth - 2-3 implants, with an edentulous upper or lower jaw - 4 implants per bar overdenture or 6-8 implants per fixed denture.10. What is the latest technology in dental implants?
Today, surgical navigation systems allow conducting implant surgery without incision using 3D modeling.This service is provided by doctors:
Book online